What is LAM?
Lymphangioleiomyomatosis (lim-FAN-je-o-LI-o-MI-o-ma-TO-sis), or LAM, is a rare lung disease that affects women almost exclusively. LAM is characterized by an abnormal growth of smooth muscle cells, especially in the lungs, lymphatic system, and kidneys. Abnormal growth of these cells can lead to loss of lung function, accumulation of lymph rich fluid in the chest and abdomen, and growth of benign tumors in the kidneys.
It is estimated that for every million women, three to seven will have LAM. However, a 2023 study of four European countries suggests the prevalence is at least 21 cases per million women– substantially higher than prior estimates. All races are affected and women with LAM have been identified in more than sixty countries. The average age of women at the time of diagnosis is approximately 35 years old. Most women with LAM have had symptoms for several years before ultimately being diagnosed.
When you breathe, oxygen passes through the airways to tiny air sacs (alveoli) in the lungs where oxygen transfers into the blood through tiny blood vessels called capillaries. The LAM cells (abnormal smooth muscle cells) cause blockage of the small airways and damage the lung tissue, reducing airflow and oxygen absorption in the blood. Scientists are working to understand the mechanisms at work in the lung that cause formation of cysts and lung destruction.
Symptoms
Some women with LAM have no or very mild symptoms, while others experience more significant indications from the beginning. Common ailments include shortness of breath, fatigue, chest pain, cough, and abdominal bloating.
Progression & Survival Rate
LAM’s progression is different for everyone. For some women, the disease progresses slowly, while for others, it advances rapidly. In all cases, lung function tends to decrease over time. Premenopausal women have a faster rate of lung decline than do post-menopausal women. Many LAM patients will, at some point, require oxygen therapy.
The median survival of patients with LAM is estimated at more than 20 years after diagnosis, with a transplant-free survival probability of 94% at 5 years, 85% at 10 years, 75% at 15 years, and 64% at 20 years.
Complications
Pneumothorax (Collapsed Lung)
A pneumothorax is common in LAM, with about three-quarters of women having at least one pneumothorax during the course of the disease. A pneumothorax occurs when a cyst bursts and air leaks into the pleural space around the lung. Symptoms usually include chest or shoulder pain associated with breathing, and a rapid increase in breathlessness. For many women, it is the first sign of LAM.
Kidney Angiomyolipomas
These are benign fatty (non-malignant) tumors in the kidneys. Angiomyolipomas occur in most patients with TSC-LAM and around 30-40% of those with sporadic LAM. Most are small and don’t cause symptoms, but they can bleed, particularly those over 4cm in diameter, requiring intervention. They can be detected by CT scan, MRI scan, or ultrasound.
Lymphatic Involvement
Although less common, LAM cells can block lymph flow causing milky fluid (chyle) to collect in the chest, pelvis, and abdomen, These are referred to as chylous pleural effusions (fluid around the lungs) and angioleiomyomas (chyle in the abdomen or pelvis). Occasionally some chyle is coughed up as sticky, whitish substance. Lymphatic manifestations occur more frequently in patients with sporadic LAM (approximately 30-40%) as compared to 10% for TSC-LAM. Drainage might be needed to confirm the chylous nature of the fluid or to relieve symptoms of shortness of breath and abdominal discomfort.
Diagnosis
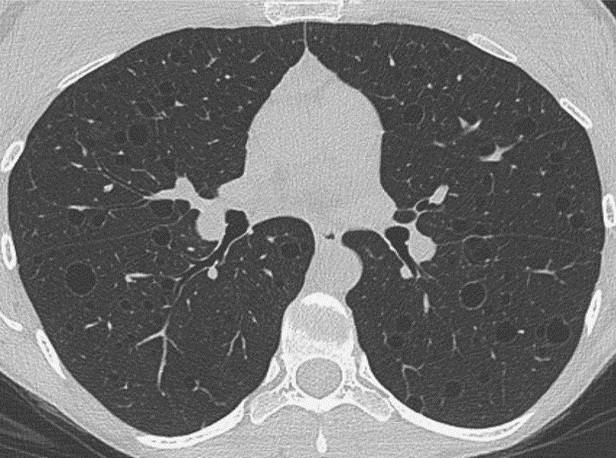
LAM presents in a wide variety of ways, making it difficult to diagnose. This is compounded by the fact that many of the symptoms of LAM are similar to those of other lung diseases such as asthma, emphysema, and bronchitis. When cystic changes in the lung that are compatible with LAM are found on a high-resolution chest CT (HRCT), the goal is to establish a LAM diagnosis using the least invasive means possible. The CT findings alone are not sufficient to confirm LAM. The presence of cystic lung disease plus the additional presence of any one of the following is sufficient to confirm LAM without requiring a lung biopsy: tuberous sclerosis complex (TSC), a renal angiomyolipoma or lymphangioleiomyoma, chylous effusions or an elevated VEGF-D level (serum vascular endothelial growth factor D), a LAM-related protein in the blood. In patients where these non-invasive means fail to provide a confirmed diagnosis, a lung biopsy may be required.
Treatment
Sirolimus
Although there is no known cure for LAM, the drug sirolimus (also known as rapamycin, brand name Rapamune) is the first-line treatment option for LAM patients with abnormal or rapidly declining lung function, substantial disease burden, problematic chylous effusions, and kidney angiomyolipomas. Studies are underway to determine the impact of starting sirolimus therapy early in the disease and at a lower dose to slow disease progression. Patients with suspected LAM or a confirmed diagnosis should be referred to a pulmonary specialist or LAM Clinic with experience using sirolimus for appropriate assessment, treatment, and monitoring.
Inhalers
Many women with LAM find that bronchodilator inhalers such as albuterol help to reduce breathlessness. Longer-acting bronchodilators are often prescribed. Some inhalers contain two long-acting bronchodilator drugs with different mechanisms of action; one benefit is that such inhalers only need to be taken once a day.
Supplemental Oxygen
When breathlessness becomes more troublesome or oxygen levels fall upon exertion or while sleeping, supplemental oxygen may be prescribed. Supplemental oxygen can be delivered from oxygen cylinders or from a machine called a portable oxygen concentrator (POC), which extracts oxygen from the air. Small, easily portable oxygen systems are also available which help people remain active.
Supplemental Oxygen GuideLAM and Tuberous Sclerosis Complex (TSC)
Tuberous sclerosis complex (TSC) is a multi-system genetic disease caused by mutations in the TSC genes, TSC1 and TSC2. LAM occurring in patients with underlying TSC is called TSC-LAM. LAM can also occur sporadically in women who do not have TSC, due to somatic mutations of the TSC2 gene. LAM not associated with TSC is known as sporadic LAM or S-LAM. Most women presenting with symptomatic LAM have sporadic LAM. Sporadic LAM cannot be inherited or passed on to children.
Occasionally people with TSC have a very limited form of the disease and few medical problems, so their TSC diagnosis may be overlooked or missed completely. For these reasons some women with LAM may need genetic tests to ensure they do not have a mild form of TSC in association with LAM. The inherited nature of TSC is very relevant when considering pregnancy since 50% of children will inherit TSC.
LAM and PregnancyThis content was created for general informational purposes only. The content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.